CSB346H1 Study Guide - Summer 2018, Comprehensive Midterm Notes - X Window System, Wireless Access Point, Vomiting

CSB346H1
MIDTERM EXAM
STUDY GUIDE
Fall 2018

Lecture 1
Lungs are the only organs which need the brain to function (heart, kidney, liver are almost independent of the brain)
When breathing fails = SIDS, sleep apnea
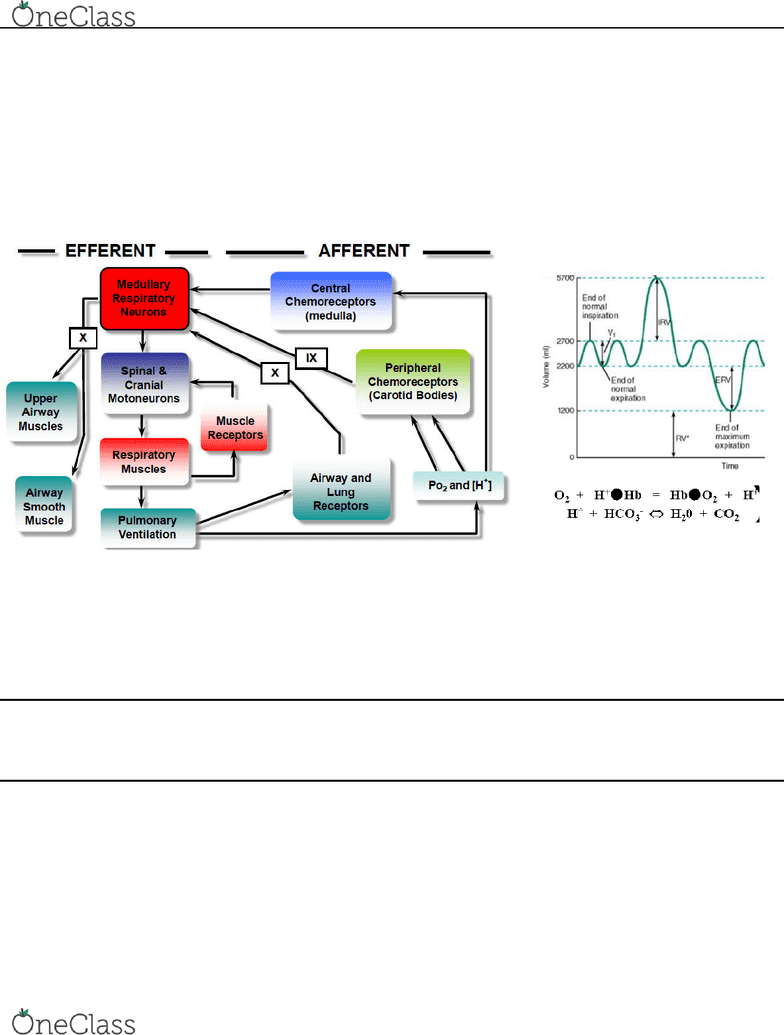
Central Regulation of Breathing
• Medullary respiratory neurons control rhythm of breathing (DRG + VRG, PRG controls shape of breathing) → X to upper airway muscles and smooth airway muscles
• Spinal respiratory motoneurons control respiratory muscles
• Respiratory muscles control pulmonary ventilation
• Muscle receptors feedback to spinal respiratory motoneurons (mechanical feedback)
• Pulmonary ventilation lungs inflate/deflate
• Upper airway muscles keep airway open while breathing (controlled by cranial nerve X)
• Smooth airway muscles
• Airway/lung receptors (mechanoreceptors throat/lungs) → X to medullary respiratory neurons
• PO2 and [H+] → peripheral chemoreceptors (carotid body) → IX to medullary respiratory neurons
→ central chemoreceptors (medulla) → to medullary respiratory neurons (ONLY pH/[H+])
Feedback Regulation of Breathing
• 2 locations: peripheral chemoreceptors + central chemoreceptors
• peripheral chemoreceptors can sense PO2 (partial pressure of O2) + pH ([H+)]
• peripheral chemoreceptors communicate with medullary respiratory neurons via the IX (glossopharyngeal) cranial nerve
• central chemoreceptors can sense pH ([H]), but NOT PO2
• central chemoreceptors communicate with medullary respiratory neurons
Vagus (X) cranial nerve (1) upper airway muscles (2) smooth airway muscles (3) feedback from airway/lungs about air volume
Glossopharyngeal (IX) cranial nerve (1) feedback of information from peripheral chemoreceptors (on PO2 and pH)
Pulmonary mechanics how lungs are inflated, how pressure from atmosphere into blood drives O2 influx
Lung volumes/alveolar ventilation how change in volume is changing metabolism
Gas transfer how O2 enters lungs from the atmosphere
Gas transport how O2 and CO2 are transported by the blood to the body
Functions of the Respiratory System
1. pulmonary ventilation ventilating the lungs (inspiration/expiration of air in the lungs)
2. gas transport & gas exchange getting O2 and CO2 from lungs and transporting into the blood (transport by hemoglobin | exchange at the tissue)
3. acid-base balance pH control ~7.4 physiological pH, through HCO3- bicarbonate ion and H+ balance
4. speaking/vocalization
5. immune protection 1st defense against toxins in air is respiratory system e.g. sneezing, secretion of mucous, immune cells and macrophages in the lungs
6. regulating body temperature important for animals that cannot sweat, panting gets rid of hot air in lungs
find more resources at oneclass.com
find more resources at oneclass.com
Diagram
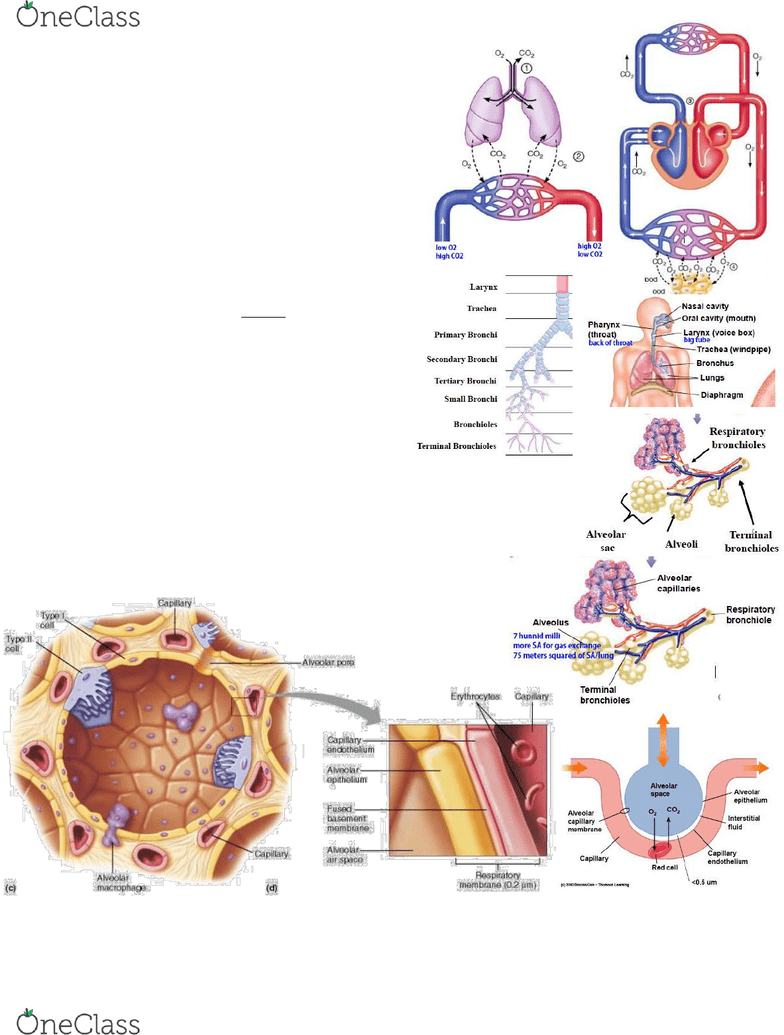
1. pulmonary ventilation 2. gas exchange (diffusion) 3. gas transport (by hemoglobin) 4. gas exchange (at the tissue)
Respiratory System Anatomy
no gas exchange at tubing, only at alveolar sacs
• Nasal cavity
• Oral cavity
• Pharynx
• Larynx
• Trachea dead space, no gas exchange
• Bronchus priary rohi, seodary , tertiary , sall , rohioles dead space
• Terminal bronchioles dead space
• Respiratory bronchioles (have some alveoli on walls) not dead space
• Alveolar ducts
• Alveolar sacs (gas exchange here)
• Alveolus/alveoli (7 hunnid milli, more SA for gas exchange, 75 m2 of lung SA)
• Alveolar capillaries (look like a sheet of blood on alveoli)
Alveoli Anatomy
2 types of alveolar cells = type 1 + type 2
Less space between alveolar epithelium and capillary endothelium = more diffusion of O2 and CO2
• Type 1 alveolar cells endothelial cells, make walls of alveoli
• Type 2 alveolar cells cells with villi, secrete surfactant to maintain alveoli shape
alveoli will collapse without surfactant due to reduced surface tension
no type 2 cells, no surfactant, alveoli collapse, cannot breathe properly
(e.g. in premature babies that do not produce enough surfactant)
• Alveolar macrophages immune cells, clean bacteria/dust/viruses
• Capillaries
• Alveolar pore
• Capillary endothelium
• Interstitial fluid
• Alveolar epithelium
• Fused basement membrane contains interstitial fluid
• Alveolar capillary membrane = blood-air barrier, only allows small gas molecules
• Alveolar air space inside of alveoli
• Erythrocytes red blood cells, have no nucleus
Blood-Gas interface
• capillaries around alveoli are so small, only one red blood cell can pass at a time
• optimizes gas exchange
• space between alveolar wall and capillary wall contains interstitial fluid
• RBCs with low O2, O2 will diffuse through walls, into RBC
• CO2 released, will diffuse through walls
find more resources at oneclass.com
find more resources at oneclass.com

